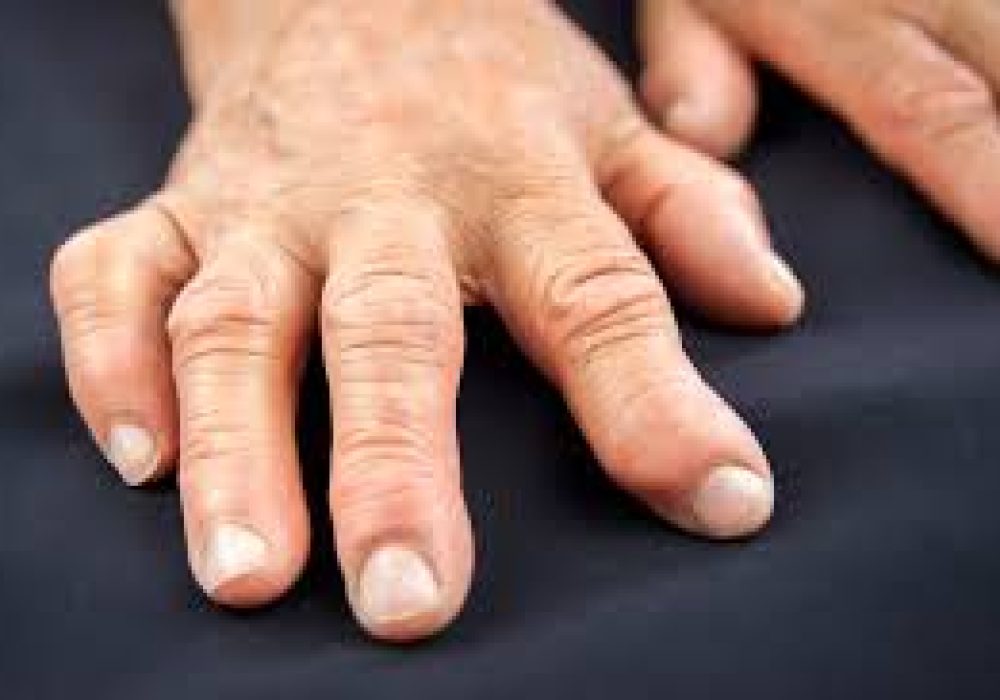
Joint Deformities: Causes, Types, Diagnosis, and Treatment
Rheumatoid Arthritis
Make Your Appointment
Joint deformities refer to abnormal changes in the shape, alignment, or function of a joint. These deformities can result from various underlying conditions, injuries, or developmental issues and often lead to pain, reduced mobility, and impaired quality of life. Understanding the causes, types, diagnosis, and treatment options for joint deformities is essential for effective management and improving patient outcomes.
What Are Joint Deformities?
A joint deformity occurs when the normal anatomical structure of a joint is altered, leading to visible or functional abnormalities. This can involve changes in bone alignment, cartilage damage, ligament laxity, or muscle imbalance around the joint. Deformities may be congenital (present at birth) or acquired due to disease or trauma.
Causes of Joint Deformities
Joint deformities arise from a variety of causes, including:
1. Congenital Conditions
Some deformities are present at birth due to genetic factors or developmental abnormalities. Examples include:
- Congenital dislocation of the hip
- Clubfoot
- Arthrogryposis (joint contractures)
2. Inflammatory Diseases
Chronic inflammation from autoimmune diseases can damage joint structures, leading to deformities. Common conditions include:
- Rheumatoid arthritis
- Juvenile idiopathic arthritis
- Psoriatic arthritis
3. Degenerative Joint Diseases
Osteoarthritis, characterized by cartilage breakdown and bone remodeling, can cause joint deformities over time, especially in weight-bearing joints like the knees and hips.
4. Traumatic Injuries
Fractures, dislocations, or ligament tears that heal improperly can result in joint malalignment and deformity.
5. Neuromuscular Disorders
Conditions affecting muscle control and tone, such as cerebral palsy or stroke, can lead to joint contractures and deformities due to muscle imbalance.
6. Metabolic and Endocrine Disorders
Diseases like gout or diabetes can contribute to joint damage and deformities.
Common Types of Joint Deformities
Joint deformities vary depending on the joint involved and the underlying cause. Some common deformities include:
1. Boutonniere Deformity
A finger deformity characterized by flexion of the proximal interphalangeal (PIP) joint and hyperextension of the distal interphalangeal (DIP) joint, often seen in rheumatoid arthritis.
2. Swan Neck Deformity
Opposite of boutonniere, with hyperextension of the PIP joint and flexion of the DIP joint, also common in inflammatory arthritis.
3. Hallux Valgus (Bunion)
Lateral deviation of the big toe with medial prominence of the first metatarsal head, causing pain and difficulty wearing shoes.
4. Genu Varum and Genu Valgum
Angular deformities of the knee where the leg bows outward (varum) or inward (valgum), affecting gait and joint loading.
5. Claw Toe and Hammer Toe
Deformities of the toes involving abnormal flexion or extension, often due to muscle imbalance or arthritis.
6. Joint Contractures
Permanent shortening of muscles or tendons around a joint, limiting range of motion.
Symptoms of Joint Deformities
Symptoms depend on the severity and location of the deformity but commonly include:
- Visible abnormal joint shape or alignment
- Pain or discomfort during movement or at rest
- Stiffness and reduced range of motion
- Swelling or inflammation
- Difficulty performing daily activities
- Joint instability or weakness
Diagnosis
Accurate diagnosis involves a combination of clinical evaluation and imaging studies:
1. Medical History and Physical Examination
The doctor assesses symptoms, onset, progression, and any history of trauma or systemic disease. Physical examination evaluates joint alignment, range of motion, swelling, and deformity characteristics.
2. Imaging Studies
- X-rays: Provide detailed images of bone alignment, joint space, and deformities.
- MRI: Useful for assessing soft tissue structures like cartilage, ligaments, and tendons.
- Ultrasound: Can evaluate joint inflammation and soft tissue abnormalities.
- CT Scan: Offers detailed bone imaging for complex deformities.
3. Laboratory Tests
Blood tests may be ordered to identify inflammatory or autoimmune causes.
Treatment Options
Treatment aims to relieve pain, improve function, and prevent progression. Options vary based on the cause, severity, and patient factors.
Non-Surgical Treatments
- Medications: Anti-inflammatory drugs, analgesics, or disease-modifying agents for inflammatory arthritis.
- Physical Therapy: Exercises to improve strength, flexibility, and joint function.
- Orthotic Devices: Braces, splints, or shoe inserts to support joints and correct alignment.
- Lifestyle Modifications: Weight management, activity modification, and ergonomic adjustments.
- Injections: Corticosteroids or hyaluronic acid to reduce inflammation and pain.
Surgical Treatments
Surgery may be necessary for severe deformities or when conservative measures fail. Procedures include:
- Osteotomy: Cutting and realigning bones to correct deformity.
- Arthroplasty: Joint replacement to restore function and relieve pain.
- Arthrodesis: Joint fusion to stabilize and reduce pain in severely damaged joints.
- Soft Tissue Procedures: Tendon release, ligament reconstruction, or contracture release.
- Synovectomy: Removal of inflamed synovial tissue in arthritis.
Rehabilitation and Recovery
Post-treatment rehabilitation is crucial for restoring joint function and preventing recurrence. It includes:
- Physical therapy focusing on range of motion, strength, and gait training.
- Occupational therapy to assist with daily activities.
- Regular follow-up to monitor joint health and function.
Prevention
While some joint deformities are unavoidable, preventive measures include:
- Early treatment of joint injuries and inflammatory diseases.
- Maintaining a healthy weight to reduce joint stress.
- Regular exercise to strengthen muscles and maintain joint flexibility.
- Avoiding repetitive joint strain and using protective equipment during activities.
When to See a Doctor
Consult a healthcare professional if you experience:
- Persistent joint pain or swelling
- Visible joint deformity or misalignment
- Reduced joint mobility affecting daily activities
- Joint instability or frequent dislocations
- Symptoms of systemic illness such as fever or unexplained weight loss
Conclusion
Joint deformities can significantly impact mobility and quality of life. Early diagnosis and appropriate management are essential to prevent progression and restore function. Advances in medical and surgical treatments, combined with rehabilitation, offer hope for individuals affected by joint deformities. Awareness and preventive strategies can also play a vital role in maintaining joint health and preventing deformities.
